Guaranteed Issue Rights also known as Medigap Protection Rights are your legal rights to purchase insurance policies when there are no open enrollment periods at Medigap. These rights prevent insurance providers from offering you Medigap insurance or requiring you to buy it. Terry Turner. Terry Turner is an independent financial journalist and Financial Wellness Facilitator. Terry Turner also covers Medicare, Social Security, and Medicare.
How do you get the benefit of the Medicare Supplement? Obtaining the Medicare Supplement plan is crucial for the retirement planning process. Medicare Supplements allow you to reduce or limit the risk of potentially high health expenses. In some cases you can get an alternative plan without having to pay any fees or fees when you are eligible. It is important to know about your Medicare Supplement guarantee period.
There are several situations where you might enroll in Medicare Supplement (Medicap) policies and do not need to ask any underwritten questions. In the case of a guarantee rights of issue, there can be several examples: How do I find a good Medicare plan in just three quick steps? Having a clear understanding of how to skip answers is also crucial.
One quarter of all Medicare recipients were covered under Medigap for coverage of their deductible, share of costs, and protection against catastrophic expenses. This issue summary gives a comprehensive overview of Medigap eligibility and explores consumer protections under federal law.
Medicare Advantage guidelines regarding guarantee rights are no longer applicable to supplemental health plans. If you lose Medicaid, you might not be allowed into Medicare Supplement plans. The eligibility varies according to your location. If a child has not reached 65 years of age then they have waited for the month of their birthday. You can now enroll for Medicare via Open Enrollment. To apply for the newest policy you must:
Guaranteed issue implies that your health insurer can't refuse coverage for any reason. If you are guaranteed issue rights then no underwriting health question can come up. If you are guaranteed issue rights for certain circumstances, then it's vital that you use our enrollment window because it won't happen again. Most Medicare patients have certain issues. The guaranteed issue right may also have a limit.
Several states have statutory guarantee rights which affect policyholders. These states-specific rules give the beneficiary the opportunity to change their Medicare plan without a deductible for the benefit. If you are using these state based guarantee rights it's important that documentation is provided. How can a Medicare Advantage-to-Supplement Plan be changed?
If your provider does not follow Medicare Supplement rules you may qualify for new insurance policies. However, you can file a complaint with Medicare. Upon acceptance of your appeal you will be granted the right to new coverage.
Medigap policy: As early as 60 calendar days before the date your coverage will end No later than 63 calendar days after your coverage ends Call the Medicare SELECT insurer for more information about your options. Find the phone number for the Medicare SELECT company. You joined a Medicare Advantage Plan or Program of All-inclusive Care for the Elderly (PACE) when you were first eligible for Medicare Part A at 65, and within the first year of joining, you decide you want to switch to Original Medicare.
Medigap availability depends entirely on state regulations, as there is no federal regulation requiring a guaranteed issue Medigap Enrollment Medicare for under-65 enrollees. The majority of the states have established regulations regarding access to Medigap coverage for this population, although they vary considerably in scope. (Click on a state on the map above to see how access to Medigap is handled in the state.).
You have a Medicare SELECT plan and move out of the plan's service area. You joined a Medicare Advantage plan when you first turned 65, and within the first year or joining, you decide you want to switch back to “original” Medicare and get a Medigap plan. You dropped a Medigap policy to switch to a Medicare Advantage plan for the first time.
A high-deductible Plan G might be available in your state. Situation 1: You have a Medicare Advantage plan. What happens: Your Medicare Advantage plan leaves Medicare or stops giving care in your area, or you move out of the plan's service area. What you can do with guaranteed issue.
HIO may receive compensation if you make a purchase from a third-party advertiser or engage with the advertiser's content. Medicareresources.org is not connected with or endorsed by the U.S. government or the federal Medicare program. * By shopping with our third-party insurance agency partners.
All Rights Reserved. Not connected with or endorsed by the U.S. government or the federal Medicare program. This is a solicitation of insurance, and your response may generate communication from a licensed producer/agent.
When can I buy Medigap? Guaranteed issue rights Search Search Print this page. Left navigation How Medicare works with other insurance Retiree insurance What's Medicare Supplement Insurance (Medigap)? Find a Medigap policy When can I buy Medigap? Buying your Medigap policy Switching Medigap policies Dropping or losing Medigap 4 steps to buy a Medigap policy Guaranteed issue rights How to compare.
You can/must apply for a Medigap policy: No later than 63 calendar days from the date your coverage ends. Note There may be times when more than one of the situations above applies to you. When this happens, you can choose the guaranteed issue right that gives you the best choice. Can I buy a Medigap policy if I lose my health coverage? You may have a guaranteed issue right to buy a Medigap policy.
Your Medicare Supplement basic benefits won't begin until your Medicare Advantage coverage ends. Situation 2: You have Original Medicare (Part A and Part B) combined with an employer group health plan or union coverage that pays after Medicare pays its share of covered costs.
You can make the change between 60 days before your Medicare Advantage coverage ends but no later than 63 days after it ends. Group Health Plan Ends If you have Original Medicare and union or employer group health coverage that is ending, you can buy a Medigap policy.
This process is called medical underwriting. There are two situations where you won't be subjected to medical underwriting when applying for a Medicare Supplement insurance plan. The first situation is during your Medicare Supplement Open Enrollment Period (OEP), which lasts for six months and starts when you are both 65 or older and enrolled in Medicare Part B.
But you must purchase it within 63 days of the date coverage ends. Medigap Insurer Breaks the Rules If a company violates rules or regulations or if it misleads you, you can drop a Medigap or Medicare Advantage plan. You can purchase certain Medigap plans sold in your state by any insurance company.
Variations of Medigap. Several federal and state laws have made switching between Medigap plans and Medicare easier for those over 65 to take advantage of Medigap programs. In New Jersey or Connecticut, Medicare is available year round with a yearly guarantee to enroll in Medicare.
A health plan requirement that must allow people to enroll no matter whether they are old or ill; a condition in which health status is determined. In other states, the guarantee issue is free and does not affect your ability to pay for an account.
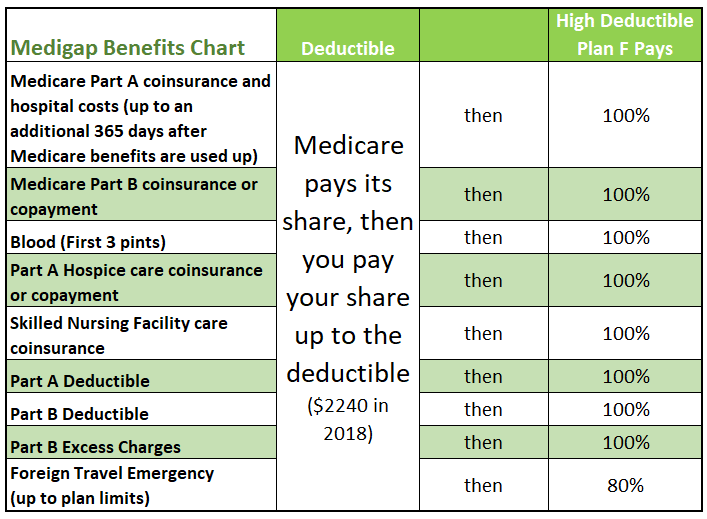
Medicare Supplement Plan F is the most comprehensive Medicare-covered plan and provides Medicare-covered care for 100% after Medicare pays a portion.